Knowing how to calculate one’s insulin sensitivity factor is a crucial skill for those who have diabetes. Here is everything you need to know about the insulin sensitivity factor and how to use it right.
RELATED: Insulin Resistance | How to Control Insulin Resistance
Insulin Sensitivity Factor | Everything You Need to Know
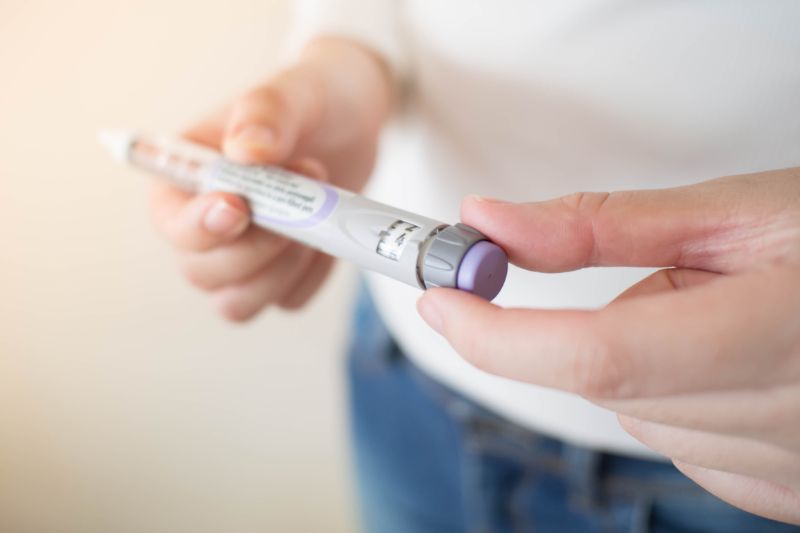
What is Insulin?
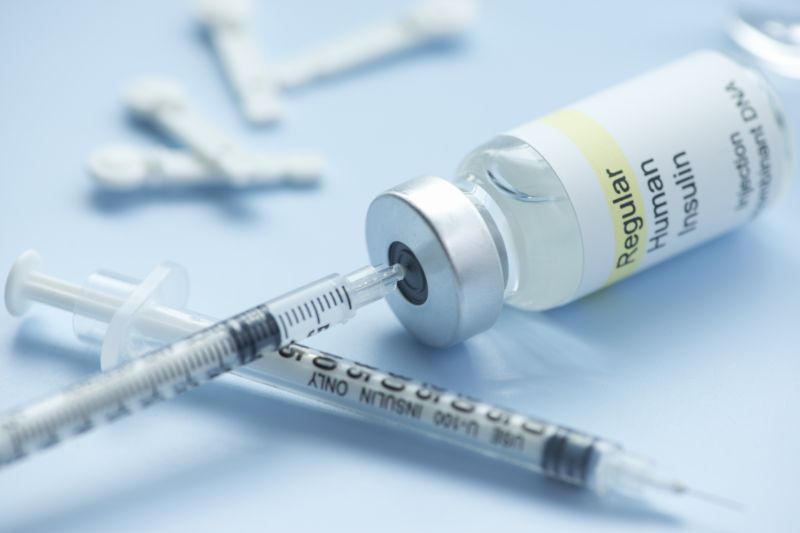
Insulin is a hormone that helps manage the body’s blood sugar levels. People who have diabetes either have no insulin or low levels of the hormone. This essentially means that their bodies are unable to process sugar or glucose in the same way that most people can.
The pancreas’ beta cells produce the hormone insulin. After eating, this hormone is released into the bloodstream, enabling the body’s cells to absorb sugar from the food, process it, and convert it to energy.
Insulin functions to store that sugar as glycogen in the liver. When the body needs energy or when its blood sugar levels are low, the liver releases glycogen from its stores.
The hormone is crucial for a person to be able to regulate his or her blood sugar. It helps ensure that the level of blood sugar does not rise too high or fall too low from its limits.
A person with type 1 diabetes is completely unable to produce insulin. On the other hand, those with type 2 diabetes still manage to produce insulin, but their bodies are unable to use the hormone properly. In both cases, it is necessary for the person with diabetes to take insulin.
What is Insulin Sensitivity Factor?
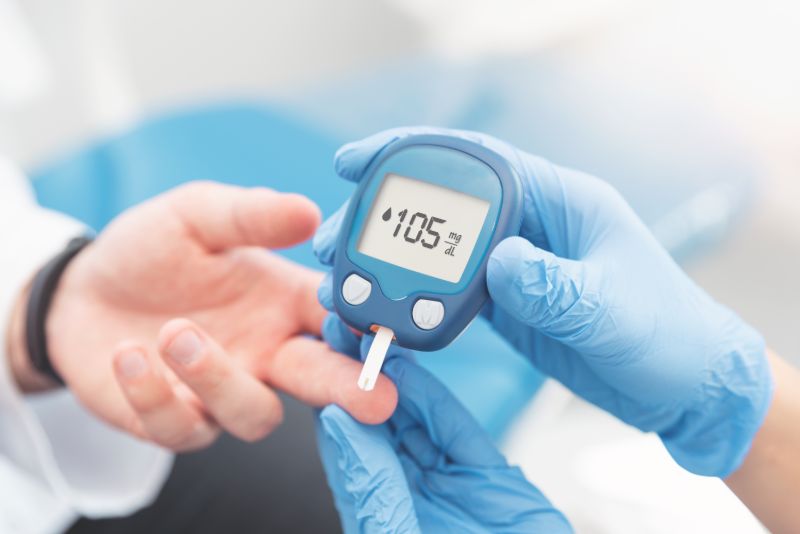
Simply put, the insulin sensitivity factor is the amount by which the levels of blood sugar of a person fall upon taking a single unit of insulin. Otherwise known as the correction factor, the insulin sensitivity factor is measured in milligrams per deciliter (mg/dL).
Understanding how to get the insulin sensitivity factor right is crucial to people with diabetes for two main reasons.
First, taking a dose of insulin that is too high can cause blood sugar levels to drop below the critical amount of 70 milligrams per deciliter. This may cause you to develop hypoglycemia and may lead to loss of consciousness or seizures.
On the other hand, taking a dose of insulin that is too low will not help your body in stabilizing its glucose levels. This results in the opposite condition called hyperglycemia, which, if prolonged, can cause a number of complications that typically affect the kidneys, eyes, nerves, heart, and other organs.
Insulin sensitivity will always differ from one person to the next. As such, it is important for those who have diabetes to understand the correct dose to take.
Generally, type 1 diabetes has a higher insulin sensitivity compared to type 2 diabetes. Furthermore, insulin sensitivity has a tendency to vary during the day depending on the person’s hormone secretion and level of activity.
When Should You Test Your Insulin Sensitivity Factor?

Insulin levels vary during the day for a number of reasons. Because of this, it is crucial to know when the best time is for you to test the factor and get the most accurate results. In general, doctors recommend testing when:
- Blood glucose goes above the target level by at least 50mg/dL
- You have not taken a dose of bolus insulin for the past 4 hours.
- You have not eaten for the past 4 hours and will not eat for the next 4 hours.
Furthermore, testing for the insulin sensitivity factor during the conditions listed below will most likely yield inaccurate results:
- You have recently had periods of low blood sugar levels.
- You are sick or emotionally stressed.
- You have just finished with strenuous physical activity.
RELATED: How to Increase Insulin Sensitivity Naturally | 9 Natural Ways to Improve Insulin Sensitivity
How do You Calculate Your Insulin Sensitivity Factor?

Calculating insulin sensitivity factor can be done in two different ways depending on the type of insulin you are using. The first method tests your sensitivity to regular insulin, while the second tests your sensitivity to short-acting insulin.
Regular insulin
This synthetic hormone begins working within 30 minutes to 1 hour after intake. The medicine then takes around 2-4 hours before it achieves its maximum effectiveness, which then lasts for about 6-8 hours.
For regular insulin, always remember the “1500 rule.” This tells you exactly how much your blood sugar levels are expected to drop for every unit of regular insulin.
If a person takes 30 units of regular insulin on a daily basis, for example, he or she then has to divide 1,500 by 30, which would give an answer of 50. This means that his or her insulin sensitivity factor is 1:50, meaning a single unit of insulin lowers that person’s blood sugar by 50 mg/dL.
Short-acting insulin
This particular kind of insulin takes much less time to affect the person’s glucose levels. After use, it takes about 30 minutes before it starts to work. After 2-5 hours, it achieves its maximum effectiveness, which then lasts for about 6-8 hours as well.
When it comes to short-acting insulin, the “1800 rule” is key. Similar to regular insulin, the “1800 rule” tells you exactly how much the body’s blood sugar levels will drop for every unit of short-acting insulin.
If a person takes 30 units of short-acting insulin on a daily basis, then he or she has to divide 1,800 by 30, which will give him or her 60. As a result, that person’s insulin sensitivity factor is 1:60, meaning a single unit of short-acting insulin lowers that person’s blood sugar by about 60 mg/dL.
How Do You Determine Insulin Dosage?
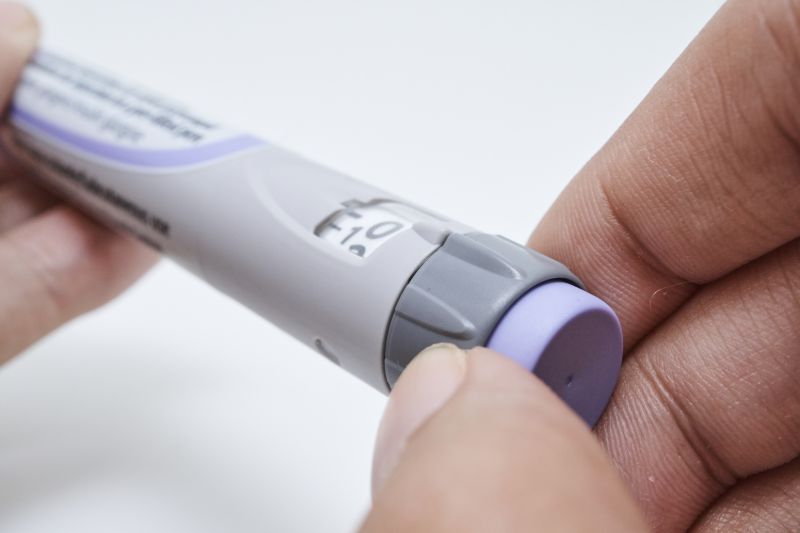
Once a person knows his or her insulin sensitivity, it is easy to figure out exactly how much insulin is needed for him or her to lower his or her blood sugar by a certain amount.
For example, a person tests his blood sugar levels and finds it at 200 mg/dL. He or she then wants to take short or rapid-acting insulin to get it down to 125 mg/dL. This means that the person needs his or her blood sugar to go down by 75 mg/dL.
Using the insulin sensitivity factor, the person knows that his or her rapid or short-acting insulin sensitivity factor is 1:60 (a unit of short-acting insulin lowers blood sugar by 60 mg/dL). So how much does the person need for him or her to get his or her blood sugar down by 75 mg/dL?
To compute for this, he or she simply needs to divide 75 mg/dL (the amount of mg/dL he or she wants blood sugar levels to go down by) by 60 mg/dL (that person’s insulin sensitivity factor). This will give an answer of 1.25.
This means that he or she needs to take 1.25 units of rapid-acting insulin for his or her blood sugar levels to go down by 75 mg/dL.
Keep in mind, however, that these are only rough calculations used by people who have type 1 diabetes. For those with type 2 diabetes, it is still best to consult with a physician for proper guidance.
Now that you are done learning about insulin sensitivity factor, take a look at this in-depth look on exactly how insulin works with this video courtesy of Novo Nordisk:
Knowing all about insulin sensitivity factor is important not just for people with diabetes, but also for their families. Learn all about this, how to calculate for it, and exactly when you should and should not test for it with the guide above.
Sorry, there are no polls available at the moment.
Do you have other questions about the insulin sensitivity factor? Ask them in the comments section below!
Up Next:
- Top 10 Diabetes Herbal Treatments From Around the World
- In-Depth Look at Type 2 Diabetes Symptoms and the Effect on Men’s Health
- Can Expired Food Kill You? 13 Expired Foods That Can Kill You
Please stay connected with us on Facebook, Pinterest, Instagram, and Twitter. Join our community here and Feel Better, Look Better and Live better with us.


